7:30 a.m., Wednesday, April 5: Yesterday I was discharged from hand rehab with John at The Institute for Hand and Upper Extremity Rehabilitation. My hand strength in my right hand is stronger than my left hand, so even though my pinky doesn’t quite have all the functionality it should, John thinks with proper use and exercise at home I can handle recovery.
As John said, implying that he could trust me to monitor and invest in my own hand health, “with everything you have on your plate, this is a mere flesh wound.”
Indeed.
With that, I had my last session of rolling and smashing silly putty and twirling balls in my hand. Really, hand therapy is not that far from children’s play. As an adult, there’s not enough activities that involve silly putty.
After a weekend of high blood pressure, my body suddenly feels low– and my blood pressure is on the low side, even after coffee, and I’m light-headed and feel as if my blood sugar could be low, despite snacking on a slice of fresh pizzeria pizza (I found that real pizza versus Dominoes or frozen varieties does not have the sodium and preservatives that impact my numbers) when I took my evening dose of Lopressor. I ate breakfast, and that helped some, but not enough. I also had an 8-ounce glass of water.
So, as my primary care doctor is signing off on me returning to work on Monday and we’re still waiting for my cardiologist’s report, I’m terrified that something might happen today. But I don’t want to manifest my own misfortune. It’s interesting to note that today was supposed to be my first day back to work, but I still have physical therapy during the day this week, and I felt better knowing my cardiologist should have the info he needs by then in case we need to make adjustments to my treatment plan.
The manufacturer of the Zio sent a push notification to my phone that they received my device and will have the data to my doctor soon.
My left hip, according to my physical therapist, was tight Monday, and now my right hip is giving me issues, the kind of issues it often has when compensating for the left hip.
I should have taken a shower last night, but I thought it would be nice to shower in the morning, but then I remembered I have physical therapy and the gym today… but I might have to take two showers today. I need to see if I can shake this feeling of brain fog and lightheadedness. By then, it will be 8 a.m. and I can call my doctor’s office. They are next door to physical therapy so maybe one of the medical assistants can take my blood pressure. Because my neurologist would be mad at me if I ignore this.
8:20 a.m. After a hot shower and exposure to The Teenager’s work drama– not being able to get into a client’s house to feed the dog– my blood pressure is now high. So I don’t know whether to call the doctor or not. I put on my sports bra inside out and my shirt backwards.
8:30 a.m. I called the doctor’s office. They won’t let a nurse or medical assistant take my blood pressure because they would like a doctor there because of my history. I have an 11:15 a.m. appointment, directly after my physical therapy, with one of the residents, I think, because it says my doctor’s name but that’s not what she told me. But it usually shows the resident’s names so we’ll see.
9 a.m. I decide to play with the Stitch Fix style algorithm before leaving as I only have a couple minutes. This will be important later… because brain fog. That was another symptom I’m struggling with– I put on my sports bra inside out and my shirt backwards.
Brief interlude while I am thinking of it. My hospital EOB came yesterday, as did updates as to some of my other medical visits. It’s obscene to see the battle between medical providers and private insurance companies. When did this become an acceptable model of business? The hospital charged my insurance company almost $18, 500 for one day of services. The insurance company pays a pre-negotiated rate of $2,500 and I get bill about $300.


In a similar fashion– the medical office billed the insurance company for the resident who so patiently spent 30 minutes removing three stitches from my face. It was itemized as “surgery” and the provider billed $66, of which the insurance company paid $13. And left $1.50 for me. So this poor resident, who worked her way through medical school and had to dig the stitches out of my scabby face, isn’t even worth $30/hour?
9:40 a.m. I arrived at Physical Therapy to sit and read my book until my appointment. Yesterday, I finished Susie Bright’s How to Read/Write an Erotic Story and I have every intention of finishing Suzanne Mattaboni’s Once in a Lifetime today.
10 a.m. or there-abouts: physical therapy with Jimmy, instead of Eric, because it’s Eric’s birthday, and his colleagues suggest that this might not be his first thirtieth birthday. I am also informed that the goal today is to poke fun at Eric as much as possible because he’s not there to defend himself.
Summary of Physical Therapy: I worked hard and found myself pushing and having good balance despite the issues with my quasi-lightheadedness. As usual, my left side is tighter than my left, but I notice as the day goes on my discomfort on the right seems to be correcting itself.
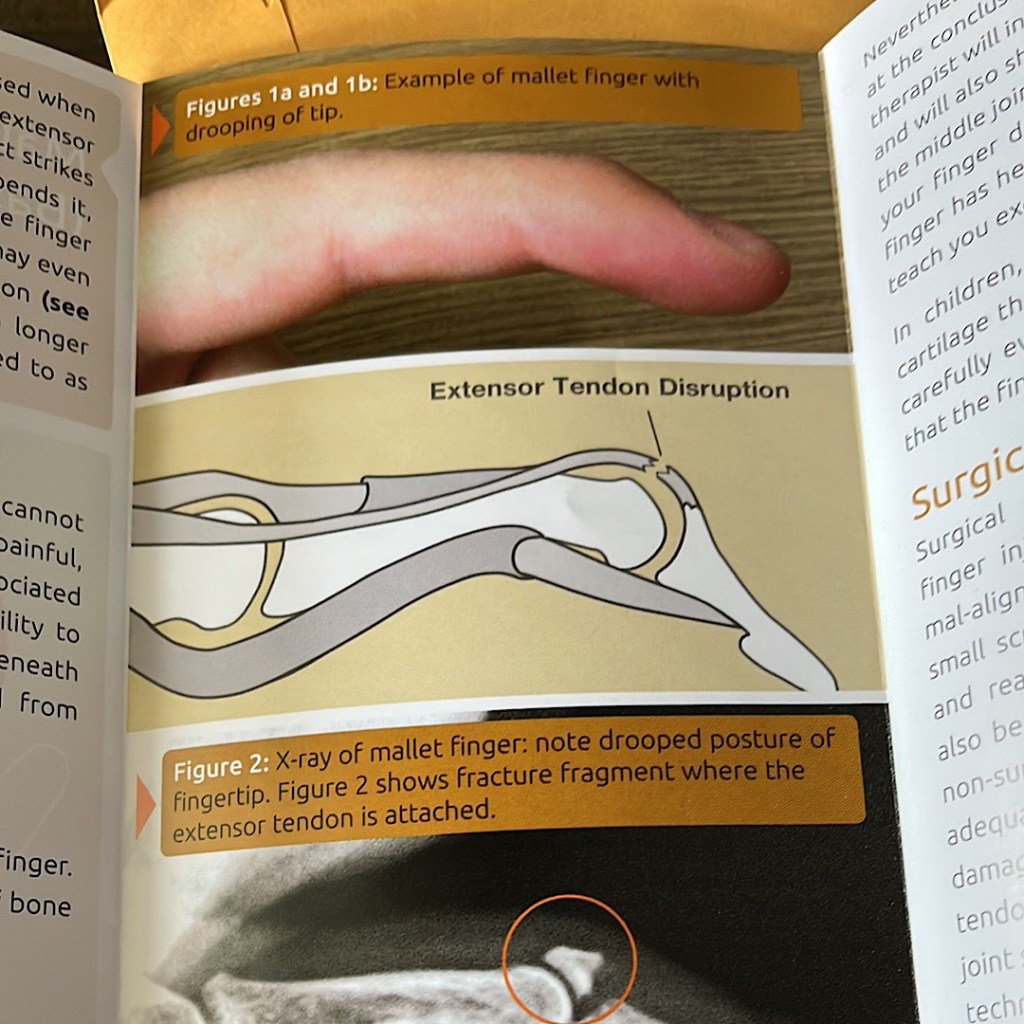
I also told my physical therapist about The Institute for Hand and Upper Extremity Rehabilitation and my mallet finger that I did last year, right before Easter. I explained how I ruptured the tendon pulling my socks off. He’s now afraid to take his socks off.
10:40 a.m. I stop at the car to update my notes and drink some water. This massive Audi SUV is parked next to me, requiring that I turned sideways to slip into my car. I take my blood pressure: 122/71.
10:50 a.m. I walk down to the primary care office, and finally put the facts together that between the physical therapy office and the family practice, there is a pediatrician. That’s why I always hear screaming children though the wall. I use the rest room and open my book.
11 a.m. My doctor’s assistant takes me back to the exam room, and confirms that I will be seeing my doctor. She’s the same person I correspond with through the portal, and who fills out all my paperwork with the patience of a saint. She doesn’t weigh me and this disappoints me because I think all this healthy eating has resulted in a smidge of weight loss.
If we’re honest, I feel silly. My head still doesn’t feel right, but I’m fine… I mean I’m going to be cautious but it could be so many things: blood sugar, blood pressure, the beta blocker, allergies or even the pollution from the major industrial fire a mile away yesterday or heck even stress… but the neurologist said… Everyone in the office, including the doctor, reassured me that I did the right thing since no one wants me to fall again.
My blood pressure was 120/77, which is pretty darn close to my car reading so that proves that my monitor is reading my blood pressure accurately and the presence of the doctors does not cause my blood pressure to increase.
11:10 a.m. the assistant leaves and I open up the final pages of my book. And I finish it in five minutes.
11:30 a.m. the doctor arrives. He sees my Alpha Books J journal in my lap and starts asking questions. Then he asks why I am there– that my chart just says “high blood pressure.” I explain that no, it’s actually lightheadedness that started with low blood pressure but hasn’t abated since my blood pressure returned to normal levels, and that the neurologist made me promise not to ignore symptoms like lightheadedness.
I explain that I got out of bed a tad clumsier than usual, after ten minutes of trying to force myself up despite 9.5 hours sleep, and I just attributed it to stiff cerebral palsy legs. But as I went downstairs and turned the lights on, I realized I was a tad lightheaded.
I poured a glass of water, took my blood pressure and my meds, and made a cup of weak (for me) coffee and finished my water and had fruit and toast.
I pass the doctor my list of blood pressure readings and tell him my first of the day was 102/68, followed by 108/65 an hour later.
He peruses the list I gave him and asks, “do you have some fancy blood pressure device that takes your blood pressure every hour?”
“No,” I say. “I’m just neurotic.”
He chuckles. “It’s not bad,” he says. “It gives me data to work with. I have patients I can’t get to take their blood pressure once a day.”
“I know you’re going to ask me what happens in certain situations, so I just want to see if I can anticipate the questions so I have the answers. Like there’s definitely a difference when I eat pizza from the local pizzeria that uses real ingredients versus Dominoes.”
He mentions I should track my pulse. I told him I look at it when I take my blood pressure because the neurologist mentioned it but I haven’t written it down. I haven’t noticed anything. And I didn’t tell him about the symptom diary I started. But I did come home and add heart rate to my iPhone tracking info. I really need an Apple Watch. Okay, I want an Apple Watch, but I refuse to consider buying one until my business computer is paid off and I replenish my savings and pay off the credit card bills I ran up during this hiatus from work.
He performs some basic exams, and has the nurse take my blood pressure lying down, then sitting, then standing up. If the low pressure is caused by gravitational pull on my body, or something like that, my blood pressure will drop as I quickly force myself upright.
My blood pressure spiked (142/100) suggesting that I tensed, which I did, because the sudden movement made me feel like I was swaying. And I braced my muscles, afraid I might fall.
So, the next test in our journey through Angel’s recent career as a face-diving professional, is to half the dosage of my Lopressor. My doctor thinks he found a note made while I was in the hospital that the IV medication made me dizzy and that’s why they switched me to the oral tablets. I don’t recall this, but a lot happened that night… so I asked The Teen much later, and she said no, my memory is correct. I read the note the doctor found, and I believe, though I could be wrong, that the real problem is doctors have no skill at writing and this leads to misinterpretation. Ooooh, maybe I need to start a “Clearer Writing Styles for Doctors” workshop.
And since my echocardiogram was perfect, and he reviewed it there with me, but I’d already read it, he wondered if the beta blocker was necessary at all (ironic since he was trying to get me on blood pressure medication for the last two-plus years) and/or if the Afib was an isolated incident. I dispute this theory, because I had two unexplained, nearly identical falls within two weeks.
My doctor reduced my beta blocker in half, which meant I had to remember to go buy a pill splitter because I already have the tiniest pills I ever saw. And he also suggested taking some sort of hydration beverage into my bedroom– a G2 gatorade or a Propel– to drink before getting out of bed.
And he closed with something like, “these are the kind of things I have to tell my patients who are 70 or 80, but unlike them, you’ll listen.”
Then he asks, “when is your next appointment?”
Not until August, I reply. He looks to me in disbelief. “I want to see you before that.”
And he sends a note to the cardiologist that he reduced my beta blocker and asks him to review the data from the Zio patch. The same Zio patch that just returned to the manufacturer yesterday.
I mention I will see the cardiologist May 5, if that matters when scheduling our next rendez-vous.
“I want you to check in in the next couple days,” he directs me, “and I want to see you next week.”
“How about April 20?” I ask. “It’s in the middle of now and April 5 and I already have to take the day off for some CT scans at the hospital and physical therapy.”
I’m going back April 20, at 8:30 in the morning, to meet with one of the residents. I didn’t think to check which one.
12:10 p.m. I leave and head to my friend Maryann Ignatz’s house to bring her some books she ordered and visit.
2 p.m. CVS. The computers have gone insane. I don’t think this will impact me as I peruse the aisles. My list is simple: a better lotion for scar care, an electrolyte drink, a blood pressure monitor, and a pill splitter.
Now, I have a borrowed monitor and I’d rather have an Apple Watch connected to a wireless monitor cuff…
And the only thing on the list today I need right away is the pill splitter.
So I find one for $8.49 and I have a 40% off coupon that expires today. I also find Propel dry powder packets that go into a water bottle– I think $3.49 for ten packets. On Amazon, the already constituted Propel Water in the same flavor costs $8.38 for 12 bottles, which is 70 cents a bottle or twice the price. I even placed one of my reusable water bottles by my bed, and I picked one with a screw-on lid designed for my bike so it’s less likely to spill.
The blood pressure monitors start at $62, and the $62 one provide $10 in Extra Bucks, but I don’t want to spend that much now.
And the only lotions “better” than the ones I have at home start at $10 and the ones specifically for scars are $20.
And on top of all that, the system doesn’t really register my Extra Care card, so it says I was logged in, but it didn’t use my coupon.
I never pay full price at CVS.
And we’re not going to talk about the fact that they were sold out of jelly beans.
3:30 p.m. I make a run to the bank and take the dog for a trip to Dunkin’ for Munchkins. Oh, and the teen. I eat too many jelly munchkins, drink a cold brew and eat one of their salty processed sandwiches, their completely not-a-Grilled Cheese with their sun-dried tomatoes. Not worth the money I paid. My blood pressure does not change. I cancel the gym for tonight because I still don’t feel stable.
I come home and I cut a pill. The Teenager then insists she can do it better and that I’m sloppy.
4 p.m. I spend some time with my cockatoo, and tend to some self-care details and start laundry.
6 p.m. The Teen and I make salads with tofu nuggets and romaine and cucumbers. The Teen devours heaps of romaine and cucumber. With a homemade fresh lime dressing.
I mention to the Teen that KFC has nuggets now.
“Really, Mom?” she protests. “You expect me to eat tofu after mentioning KFC?”
And then I proceed to drop the knife several times while chopping vegetables. I’m amazed I still have all my toes. Brain fog is so real.
6:45 p.m. I text the neurologist just to update her.
7 p.m. I place my last load of laundry into the dryer and find a half pill of my beta blocker on the table.
I call the teen’s name.
“Did I not take this with dinner? Did I miss my mouth?”
“I doubt you missed your mouth,” she reassures me. “It probably just slipped out of the bottle.”
“I could count them,” I say.
“And if there is an even number, you fucked up,” she says.
It was an odd number.
7:30 p.m. I finally retire to my room hoping to start a new book as part of my pre-bed, no screens ritual. I make the bed, feed the cats, put my Propel packets in my drawer and organize my lotion (for scar massage on my finger and my face) and my water bottle. But first I have to finish this blog entry. And I notice– to my chagrin– that somehow this morning I changed my next Fix from May 18 to April 18. Hopefully I can change it back before the stylist grabs it, because my charge card needs to take a little vacation from my wallet until I rebuild my rocky finances.
And that, friends, was my day. Louise the Tripod is snuggled against me, kicking me with her back feet and snoring. I still need to give the bird water, make my Propel, brush my teeth and massage my scars. So, if you think I’ve been over here partying during this short-term disability leave, I have not.